Topical cannabis preparations have been around since the dawn of civilization and have experienced a resurgence in popularity along with medical cannabis. Usually these salves and creams, which are rubbed into the skin directly, are intended to treat conditions directly below the skin. For instance, cannabis-derived salves are popular among those suffering from arthritis, who apply the cream directly to affected areas to reduce swelling. This method of administration is believed to be more effective for arthritis than oral administration and also avoids many of the otherwise psychoactive effects of cannabis.
Of course, manufacturers of cannabis creams and salves are often liberal with claims of conditions the cream can help. For instance, some websites discuss the use of cannabis-derived cream to completely eradicate cancerous tumors or genetic diseases. At this stage of cannabis and cannabinoid research, many unknowns remain, so technically it is possible these claims are true. However, knowing what we know at this point in time, this is probably utter nonsense. To be fair, these manufacturers may have witnessed healing that happened in tandem to salve application and may honestly believe their claims. However, there is a stark difference between several personal observations about using a salve and the extensive laboratory testing needed to scientifically support those claims.
Regardless, the question remains: what can cannabinoid salves and creams be used for? As it turns out, there may be an accidental shred of truth to over-zealous claims that the salve can solve more than topical issues. Recently, the DARU Journal of Pharmaceutical Science published a paper detailing the work of a research group that examined the therapeutic potential of cannabidiol cream in mice with experimental autoimmune encephalomyelitis (EAE). EAE is an animal model of brain inflammation used to mimic human diseases such as multiple sclerosis (MS). In this general type of disease, the immune system is attacking healthy areas of the body, specifically the protective linings of neurons in the brain, which can cause physical paralysis and mental issues. For the mice in this experiment, EAE was triggered intentionally by injecting a protein that leads to an autoimmune chain reaction.
In MS in humans, once the disease damages nerves that control muscle function, many patients suffer from spasticity of limbs, as well as inability to move. By now, CBD has been thoroughly established as a neuroprotective and anti-spastic agent. In fact, it has been adopted into standard medical practice as a backup drug (known as Sativex), should patients not respond to the first line of pharmaceuticals. Sativex is a 1:1 solution of THC:CBD, the two most active cannabinoids found in cannabis. However, Sativex is applied orally; researchers wanted to know if topical administration of cannabinoid cream could have the same results, or perhaps even be more effective.
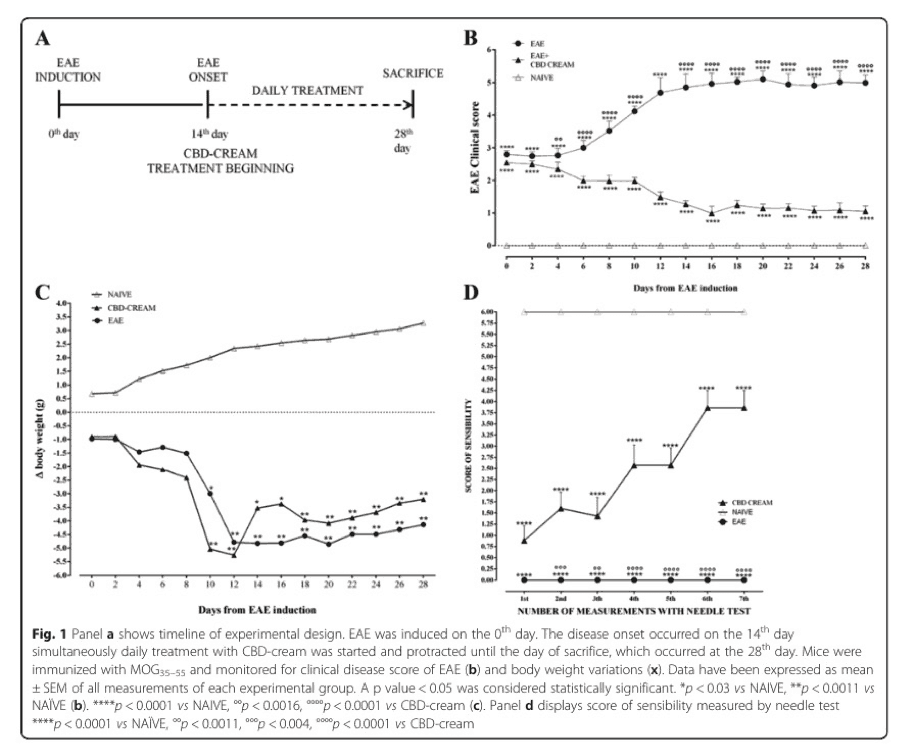
To test this, researchers separated the mice into several groups: a control group that did not have EAE, a group that had EAE disease with no treatment, and a group that had EAE disease with 1% CBD cream applied to a thigh area once every 24 hours. Scientists then recorded the progress of disease in the rodents for two weeks. Three scores were used to evaluate the acceleration of the disease: body weight, the needle test, and a clinical scale of EAE symptoms, ranked by stages of immobility. Body weight helps to serve as an indirect indicator of the disease due to the muscle loss and atrophy that occurs as limbs become less mobile. The needle test, on the other hand, helps to indicate nerve sensitivity. In that test, a needle or filament is applied with gradually increasing pressure to mouse paws. Mice receive higher scores for withdrawing their paws at lower pressures (because this means they have retained more nerve sensitivity).
The results are shown below:
While rodents without the disease obviously fared best, application of CBD cream to those with the disease was able to decrease the clinical EAE score/ranking, increase body weight, and increase paw sensitivity in the needle test. In fact, paw sensitivity was almost 3/4ths recovered and may have recovered more given a longer trial. These are excellent results, considering that in general, autoimmune diseases are not curable by currently available pharmaceuticals.
In other words, the use of a topical salve or cream could very easily have substantial neurological effects. In light of that, those suffering from autoimmune disease may benefit from trying topical cannabis preparations. This research would indicate that it’s worth a shot, and we know that there aren’t any apparent negative consequences of application. Regardless, this is not only good news for those suffering from autoimmune disease. It also hints that topical cannabinoid ointments, in general, can be formulated to affect areas of the body other than simply where they are applied. At this point in time, few pharmaceutical companies have given serious focus to producing cannabis salves and creams; the focus now is clearly on oral pharmaceuticals. However, the success of this experiment indicates that cannabis ointments may become more popular as more research is conducted. For the time being, however, we’d advise consumers to be cautious and not rely on a cream or salve as the sole treatment for any serious, life-threatening conditions.
Works Cited
Sabrina Giacoppo, Maria Galuppo, Federica Pollastro, et al. A new formulation of cannabidiol in cream shows therapeutic effects in a mouse model of experimental autoimmune encephalomyelitis. DARU Journal of Pharmaceutical Sciences (2015) 23:48.