Imagine having to re-live the worst moment of your life every time you sleep. Imagine that rather than being able to rest, you’re forced to experience that moment in slow motion over and over, feeling horribly trapped in a world you did not ask to be in. For some individuals with Post-Traumatic Stress Disorder (PTSD), this is literally the situation they face.
In the last article about cannabis and sleep, one of the major points we hoped to communicate is that sleep disorders are caused by a variety of reasons, each with its own special set of circumstances. Individuals with sleep disorders resulting from PTSD comprise one of those sub-groups and can be one of the hardest groups to treat. As we’ve discussed in previous articles, PTSD can be thought of as the brain’s attempt to help itself or to protect the individual from further harm. After experiencing something deeply disturbing and traumatic, the brain becomes overly focused on the event, constantly re-hashing, re-living, and re-dicing the situation as if it were to glean some special knowledge or produce some behavior that will prevent the event from ever happening again. Unfortunately, that’s just not how life works. Sometimes terrible things happen for no reason at all. While fully processing serious events is important and necessary in the short term, true long-term healing means the ability to leave it in the past and to avoid letting it define one’s identity. Individuals with PTSD have difficulty doing this due to brain changes from the trauma, and as a result one common side effect of PTSD is having nightmares relating to the event of trauma. These nightmares are not only mentally de-stabilizing but also cause a loss of sleep and degradation of sleep quality. As a result, individuals with PTSD may have trouble getting adequate rest, even when they feel tired.
The purpose of dreaming during sleep is not completely understood; researchers theorize that it plays a role in information processing. For healthy individuals, dreaming during sleep is generally beneficial, although for individuals with PTSD, these dreams clearly do more harm than good. An ideal supplement for those individuals then would be something that prevents dreaming during sleep without greatly reducing the quality of sleep. As it turns out, cannabis is capable of doing exactly that. Not surprisingly, many individuals with PTSD are already using cannabis for the same reason.
In a study from the National Center for PTSD, researchers investigated the uses of cannabis by patients at local cannabis dispensary. The procedure included 170 individuals who opted-in to the study and asked to complete a survey. This survey asked typical questions about cannabis and alcohol use but also included a questionnaire that helped rank the presence and severity of PTSD symptoms. That questionnaire was then scored and used to separate study participants into two groups: those with PTSD and those without. Finally, participants were given a commonly used cannabis motivation questionnaire to establish primary reasons for cannabis use. After examining the data, researchers found a strong correlation between the motivation of using cannabis to sleep and the group of PTSD-afflicted cannabis users. Individuals with PTSD are more likely to use cannabis for sleep disorder than other cannabis users.
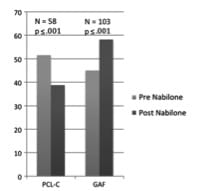
Noting this same association, researchers have warmed to the idea of using synthetic cannabinoids to more formally treat those with sleep disorders related to PTSD. In one study from the University of Ottawa, researchers analyzed a population of male inmates with serious mental illness. Researchers first took note of those who had been prescribed Nabilone at some point during treatment. Nabilone is a synthetic cannabinoid commonly used to treat chronic pain. Armed with that data, researchers then compared those inmates scores on both a commonly used metric for assessing PTSD (seen as PCL-C on the graph below) as well as a metric used for measuring general mental health (seen as GAF), both before and after receiving Nabilone.
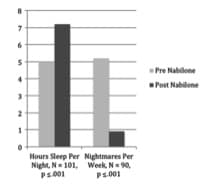
As the results showed, patients showed improvements in two areas as a result of taking Nabilone. First, patients showed an increase in self-reported hours of sleep and a reduction of total number of nightmares per week. Secondly, patients scored lower on the PTSD assessment, indicating less expression of PTSD, as well as higher on the general mental health survey.
(Graph 1 Inset: Graph showing hours of sleep and nightmares per week both pre- and post-Nabilone treatment)
(Graph 2 Inset: Graph showing PCL-C and GAF scores both pre- and post-Nabilone treatment)
Based on these results, cannabis and more specifically the endocannabinoid system show great promise for the treatment of PTSD-related sleep disorders. The caveat to this current research is that both studies relied on self-reported information, which gives us a limited picture of the relationship between PTSD and cannabinoid treatment. However, as research about cannabinoids continues to grow and stigma related to cannabis-use simultaneously decreases, we hope to see more and more availability of cannabis or cannabis-related treatments for those suffering with PTSD. In the meantime, we would encourage those suffering from PTSD nightmares to give treatment with cannabis a try to determine if use is helpful on an individual level.
Works Cited
Marcel O.Bonn-Miller, Kimberly Babson, and Ryan Vandrey. (2013) “Using cannabis to help you sleep: Heightened frequency of medical cannabis use among those with PTSD”. Drug and Alcohol Dependence (2014) 136:162-165.
Colin Cameron, Diane Watson, and Jeffrey Robinson. (2014) Use of a Synthetic Cannabinoid in a Correctional Population for Posttraumatic Stress Disorder Y Related Insomnia and Nightmares. Journal of Clinical Psychopharmacology (2014) 34: 559-564.