The last time we spoke of opioids and cannabis, it was in reference to whether cannabis could interfere with opioid withdrawal recovery (spoiler alert: not observed). However, equally worth considering is the opposite end of the spectrum of opioid users: legitimate use of prescribed opioids to treat chronic pain. Noting the tendency for opioids to be abused and to elicit addiction in patients, doctors must be very careful about prescribing opioids and must gauge a variety of factors such as age and tolerance to pain. However in almost all cases, patients receiving opioids have tried other less potent painkillers, from over the counter to prescribed medications, and have not had success with these medicines. Unfortunately, while opioids represent one of the strongest painkillers known at this time, they have not been shown to be effective in managing chronic pain. Furthermore, our current medical understanding of pain is that it cannot simply be reduced to one factor or one area of the brain. As a result it is unlikely that one substance will contain the entire mechanism of action for eliminating pain. This dovetails nicely into cannabis use because as we’ve discussed on the blog previously, cannabis is capable of activating pain attenuation circuits through the endocannabinoid system. Specifically, cannabis can activate some of the same opioid pathways without actually supplying extraneous opioids to the body.
Those that read the blog know that a pet peeve of Cornerstone is seeing small studies. We like to see large studies upwards of a thousand subjects that cut across all sectors of society. Unfortunately, we rarely get that joy, as cannabis research is only recently being considered seriously on a large scale. Researchers also generally have an easier time accumulating small studies. Asking the question of how effective cannabis use can be at attenuating long-term pain can therefore be difficult on a large scale. One group, however, the National Drug and Alcohol Research Centre of Australia came up with a very clever way of looking at this phenomenon. In this study, researchers contacted roughly 93% of community pharmacies in Australia, asking them to note customers receiving prescription opioids. After filling those prescriptions, pharmacists were then paid to survey those customers with a specific questionnaire designed to benchmark pain and opioid treatment, called the Pain and Opioids in Treatment (POINT) study. Additional questions were added, such as those from the Pain Self-Efficacy Questionnaire and the Brief Pain Inventory. Questions about cannabis use were also administered. In total, the survey netted 1514 participants from a variety of economic and cultural groups across Australia.
Armed with this data, researchers were then able to answer basic questions about cannabis use in those with chronic pain, as well as perform statistical regression to evaluate how much cannabis use contributed to the elimination or tolerance of that pain. The first few discoveries were not surprising: participants using cannabis were more likely to have back or neck problems as opposed to arthritis, had been dealing with chronic pain for longer, and were receiving higher doses of opioids. For many of you reading this blog, this might hit close to home. You may have started with the intent to treat pain “by the book” and over time had become desperate for anything that would work at all.
Yet the most interesting point of the data is the correlation to reduced pain, even after researchers controlled for the amount of pain and dose of opioids in each patient. As seen in the table below, researchers observed an association between cannabis use for pain and pain interference (the ability to reduce that pain) with a P-value of below 0.001. Without getting into a discussion of statistics, this means that the correlation is all but certain, and given the large number of individuals observed, the study represents a strong data point in the conversation about treating pain with cannabis. Additionally, the average pain relief reported from using cannabis was 70%, while the average pain reported from using opioids was only 50%.
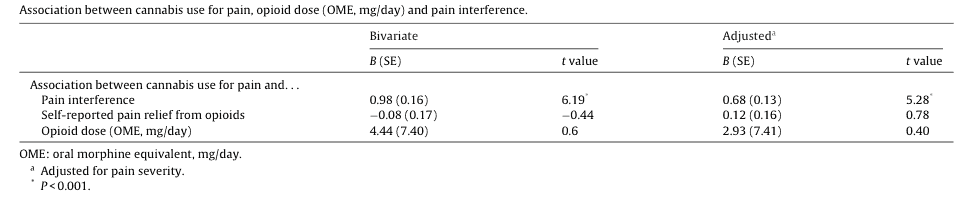 (Graph inset: A correlation between cannabis use and pain interference in individuals prescribed opioids for chronic pain is observed with a P-value of below 0.001.)
(Graph inset: A correlation between cannabis use and pain interference in individuals prescribed opioids for chronic pain is observed with a P-value of below 0.001.)
Self-reported data, of course, relies on participants being both honest and accurate about their use. A variety of reasons could exist for lying about opioid or cannabis use, particularly when using either would be illegal. However, in this case, this would likely be skewing the data to eliminate the observed effect; if participants were afraid about reporting cannabis use, then potentially some of the pain attenuation observed could be an effect of that un-reported cannabis use. Simply put, this means that the association between cannabis use and chronic pain relief is likely higher than observed.
Capping off this discussion, Dr. J. Michael Bostwick, of the Mayo Clinic, recently wrote an editorial in the General Hospital Psychiatry journal discussing the use of cannabis for management of chronic pain. In that editorial, Bostwick argued that “cannabis can – and should” – be more often prescribed for individuals with chronic pain management problems. Bostwick reviewed various studies to cite his position and also noted the potential risks of cannabis use. He was quick to point out that he is not a blind-supporter of cannabis for any situation, but considers it essential to the modern pharmacological approach to pain. While an editorial on its own is not evidence of cannabis’ effectiveness in this situation, this is evidence of a growing shift in attitudes in the medical community. As a result, we at Cornerstone expect to see more research in this area and plan to keep you up to date with the developing discussion.
Works Cited
Louisa Degenhardt, Nicholas Lintzeris, Gabrielle Campbell, et. al. (2014) Experience of adjunctive cannabis use for chronic non-cancer pain: Findings from the Pain and Opioids IN Treatment (POINT) study. Drug and Alcohol Dependence (2014) 147:144-150.
J. Michael Bostwick. (2014) The use of cannabis for management of chronic pain. General Hospital Psychiatry (2014) 36:2-3.

