One of the most important concepts that our blog can communicate to readers is that cannabis is the tip of the iceberg when it comes to understanding the endocannabinoid system. This chemical system, that happens to respond to cannabis, was not merely an afterthought in the evolution of the human body, but actually exists in many different animals as well (including birds!). Thanks to the resurgence in cannabis and cannabinoid research around the globe, new uses for the system are constantly emerging. So far, the scientific community has shown most interest in direct uses of the endocannabinoid system to formulate new medicines for stress, pain, neuroprotective effects, and metabolism. However, researchers in Finland have identified a new use of the system…as a biomarker!
Biomarkers are any indicators used to track and identify the existence of a biological state or condition. While that sounds complicated, many readers may have already benefitted from the use of biomarkers during medical procedures or checkups. For instance, those with chronic heart problems may already be familiar with the “nuclear stress test”. In this test, doctors are attempting to see how blood is being pumped through the body and which areas are not receiving enough blood during vigorous exercise or cardiac stress. Unfortunately, attempting to crack open a patient’s chest to view this directly would be dangerous, time-consuming, and costly. Additionally, even with the chest open, the doctor would have no quantifiable way to measure blood-flow in each small area. To solve this, doctors often inject patients with a radioactive chemical (typically Tc-99 or Myoview). The chemical then flows throughout the bloodstream and doctors are able to take scans with special cameras that detect only radiation (in this case, gamma rays). Since radiation will only appear where blood has carried the radioactive chemical, doctors can then literally see where blood is in each tissue. Useful right?
In the case of a nuclear stress test, the biomarker is the radioactive substance, effectively “marking” where blood is. However, biomarkers can be anything, not just radioactive chemicals, but also dyes to show color change in tissues, or even our receptors themselves. This is where the endocannabinoid system comes into play with brown adipose tissue (BAT). BAT is one of the two kinds of fat tissue found in mammals. The other kind, white adipose tissue, is what most readers will think of when they think of fat tissue, which stores energy and traps heat. As with white tissue, brown tissue also helps trap heat near the body. However, unlike white tissue, brown tissue’s primary function is to generate heat itself via constant chemical reaction, especially in animals that do not shiver. Think of it as nature’s electric blanket. As a result, it is found in large quantities in newborns (baby fat!) as well as in mammals that hibernate (much of the fat they store is BAT). As humans age, our brown fat tissue tends to turn into simple white fat tissue, because it is no longer needed. However, scientists have recently discovered that there is more BAT leftover in adults than originally thought, and as a result, scientists are working to investigate the role it plays in the body.
Of course, to investigate the role of BAT, we need a simple way to see where it is located. Researchers noticed something odd in rodent experiments; when Rimonabant (a chemical that effectively deactivates cannabinoid receptors) is applied in rodents, an activation of BAT tissue occurs. Further research has confirmed that activation of the CB1 endocannabinoid receptor specifically leads to heat production in BAT tissue. Finally, long-term loss of CB1 receptors leads to a fat conversion in the body in which white fat tissue is converted to brown, heat-producing tissue. Taken all together, this strongly suggests that CB1 receptors play an important role in BAT tissue regulation, which would mean they must be present in BAT tissue.
To test this theory, researchers first dissected rats and froze their tissues. From there, they were able to cut thin slices of tissue to mount on slides and then stain these with a fluorescent marker of the CB1 receptor. Afterwards, researchers were able to photograph the tissues and note where CB1 receptors were and were not located.
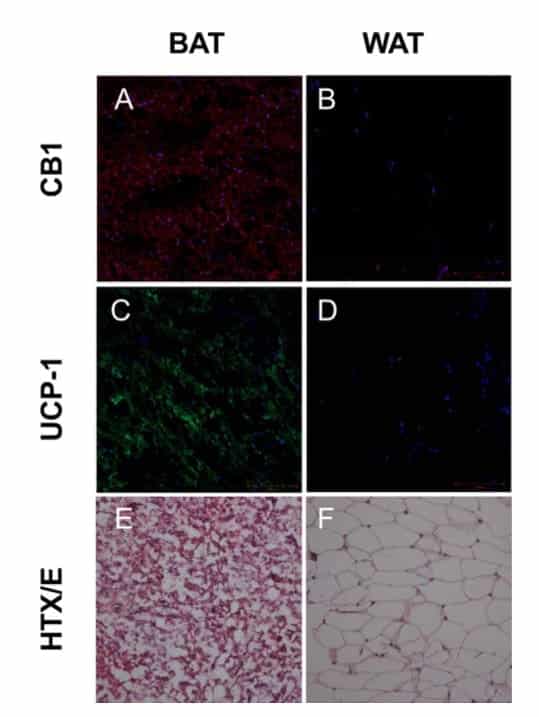
Graph inset: Pictures of fluorescent dye marking the existence of CB1 in both BAT (brown adipose tissue) and WAT (white adipose tissue).
As seen in the graph above in section A, red dye indicating the existence of CB1 receptors appears all throughout the brown adipose tissue (BAT). However, no red dye appeared in white adipose tissue (WAT), which means that CB1 receptors do not exist there. To confirm that the correct tissue was selected to represent brown and white adipose tissue, researchers also tested for a specific protein found only in brown adipose tissue, UCP-1. As readers can see from sections C and D, this protein (glowing green) was only found in BAT sections, confirming that the correct tissues had been selected.
As a result, researchers have confirmed that CB1 receptors exist only in brown adipose tissue and not in white adipose tissue.
Why is this important? Since the amount and percentage of brown to white fat varies for each human and cannot be determined externally, investigating the amount of brown adipose tissue would be difficult without surgery. However, thanks to the discovery that the endocannabinoid system can effectively serve as a biomarker, researchers now have a way to visualize brown adipose tissue; they can first inject the body with a radioactive marker that attaches only to CB1 receptors. From there, using a camera that detects radiation, they can then observe which areas of fat have CB1 receptors (and are therefore areas of brown tissue) and which do not (and are therefore areas of white adipose tissue). Further testing must be done to determine the ideal specifics of this procedure (such as which tracer and how much tracer to use), but the bottom line is that we now have a new tool for investigating brown adipose tissue.
This represents one of the great ways that endocannabinoid research is helping us to understand areas of the human body that at first glance may appear completely unrelated to cannabinoids and cannabis science. Due to the endocannabinoid system’s prevalence throughout the human body, both in the brain and in the periphery, we can expect to encounter similar situations in the future, where endocannabinoid research leads to new tools of discovery and better medical treatment options.
Works Cited
Olof Eriksson, Kirsi Mikkola, Daniel Espes, et al. (2015) The Cannabinoid Receptor-1 is an imaging biomarker of Brown Adipose Tissue. Journal of Nuclear Medicine (2015) DOI: 10.2967/jnumed.115.156422